A significant mass of a person falls on the lower back, and by lifting the load, turning, from a long static position, additional stress is created on it. Excessive load, the wrong lifestyle constantly leads to the degradation of the musculoskeletal system - the vertebrae and the discs between them, which serve as shock absorbers. From this point, it is worth looking for information on osteochondrosis of the lumbar spine: symptoms and treatment. Why does the degradation of the spinal joints occur?
The degradation of the musculoskeletal system occurs in the following way: the natural shock absorber of the spinal column loses its elasticity, shrinks, extends beyond its natural limits, the pressure of other vertebrae, organs and ligaments increasesfurther. Let us describe those who are prone to acquiring such a pathology. Osteochondrosis of the lumbar spine can be seen in people:
- whose first generations suffered a similar affliction;
- Have hormonal disorders;
- Individual propensity to develop such diseases (eg, congenital structure of the spine);
- Those who neglect proper nutrition. At the table every day, a person should be given a balanced diet with healthy fats, vitamins, proteins;
- Those who have a sedentary job: sit for a long time or stand for a long time in one place;
- Experiencing a strong and sharp load on the spine, for example: weightlifters, loaders, people during garden work;
- Having diseases of the digestion, metabolism, pelvic organs;
- Traumatized (pulled too hard on the back, hit sideways, fallen, bent over);
- Have reached 30 years of age;
- Diabetes.
If there are signs of lumbar osteochondrosis, which are described in the next section, some habits should be avoided:
- hunched over;
- smoke;
- adopt a bowed pose for a long time;
- move around a bit;
- drinks alcohol;
- sit down without taking breaks at work;
- don't dress for the weather, let the body cool down.
Important. Any disorder in the ligaments is aggravated by the presence of excess weight. With excess weight, the load on the lower body increases and the lumbar region, covered with fat, is strongly massaged.
Stages of the disease course, its signs
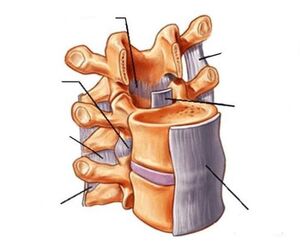
At first, there are periodic minor pains that increase with physical exertion. This discomfort suggests that it is time to pay attention to osteochondrosis of the lumbar spine. At this time, the intervertebral discs (the spinal disc is the channel through which the spinal cord and the fibrous ring that surrounds it) are degrading. In addition, the distance between the vertebrae is reduced, the nerves are pinched. The pain becomes severe, it takes over not only the back, but also the hips, the gluteal muscles. In the third stage, the fibrous rings are destroyed, which leads to the formation of a hernia of the spine, irreversible stooping, and pain is constantly present. The fourth stage leads to disability. The special classification of osteochondrosis of the lumbar spine includes:
- pain;
- ischemic syndrome;
- radicular syndrome;
- vertebral syndrome;
- ossification of overgrown tissues.
Pain sensations have a different degree and character of severity: lumbago, for example, is called lumbago; constant, aggravated by stress, lumbodynia; The spread throughout the lower parts of the body is called lumboischialgia. In the event that back diseases are not addressed, the vertebrae acquire too much free movement in the spine. There is a compression of the nerve roots when lifting loads and sudden actions, then the lower back pain goes away, but it moves to other parts of the body, for which the nerve is responsible. Unconsciously, we change position, adjusting so that the pain occurs less in the back, but at the same time the gait and the flexion of the spine inevitably change. All of this refers to root syndrome, which starts out as irritation and then becomes inflammatory. Signs of osteochondrosis of the lumbar spine with radicular syndrome:
- The back muscles are excessively tired;
- back curvature change;
- changes on the fly;
- swelling of the lower extremities;
- pain in one or both legs;
- severe pain;
- temporary loss of sensation in the legs;
- periodically prolonged constipation;
- men have excitability problems;
- menstrual irregularities in women;
- intoxication of the body;
- blood stagnation.
You may notice that during breaks, painful sensations arise, and when doing back exercises, they disappear. Already at this stage it is worth looking for a doctor - a chiropractor, surgeon, neurologist, traumatologist (since the causes of osteochondrosis of the lumbar spine include trauma). If you let the disease run its course, the problem will increase, supplemented by different companions:
- heat;
- numbness;
- sweating;
- tingling;
- chills;
- goose bumps;
- impotence;
- intestinal colic.
The back muscles lose their tone and this leads to a general loss of human motor functions. With a particularly dangerous course of radicular syndrome, paralysis will occur. Ischemic syndrome is associated with radicular. At first, compression of blood flows is periodic, but later such compression leads to spasms. You may notice them during normal walking: you walk in pain, if you stop, it doesn't hurt. The main degradation occurs inside and is not visible to the naked eye: the blood flows do not provide all the pelvic organs with the necessary supply. There may be pain in the buttocks, thighs, and later paralysis of the gluteal muscles may occur. Vertebral syndrome already includes a change in the skeleton, the blood vessels themselves.
Important. Symptoms of lumbar osteochondrosis in women are inextricably linked with the hormonal background, the physiological characteristics of the body. The appearance of pain, incorrect posture is affected by the use of inappropriate shoes: with too hard or too soft soles; too high a heel or too low a heel.
Diagnosis of disease stages

It can be very difficult even for a doctor to classify and name the stage of the disease during an external examination. Initially, a neurologist can diagnose:
- persistent curvature of the spine;
- pain when touching;
- decreased leg travel;
- asymmetry of the gluteal area;
- change the Michaelis diamond.
But the most accurate diagnosis can only be made with the results:
- computed tomography (CT). The most optimal option for determining the degree of development of the disease, which makes it possible to assess the stage of degradation of the spine.
- X-ray filming. According to them, it is possible to establish the presence of an ailment, but it is not always possible to determine the degree of development of damage to nerve fibers and blood vessels.
- magnetic resonance imaging. Quite long (half an hour to an hour), an expensive procedure, which also provides the most complete detail of what is happening with the nerve roots and blood vessels.
Therefore, the doctor can finally judge about the osteochondrosis of the lumbar spine: symptoms and treatment only with the results of the research of appliances. Low back pain, not associated with a violation of the intervertebral disc, is caused by colds, chills in the kidneys, menstrual cycle or pain in the back muscles.
Important. CT scans and X-ray exams are unacceptable for pregnant women. CT is not safe for: 1) children under 14 years of age; 2) people with an allergy to iodine.
Medical treatment
The causes of the appearance of the disease, its characteristics are considered above, now we turn to the second point of osteochondrosis of the lumbar spine: symptoms and treatment. The more you ignore the body's signals, the faster the disease will progress. The further from the beginning, the more drugs and procedures will need to be applied. Treatment objectives:
- identify, eliminate the causes of pinching the roots, the vessels of the spine;
- restore skin sensitivity;
- to prevent further development of pathology;
- initiate the body's processes for self-healing;
- strengthen a person's muscle tone;
- restore the function of the internal organs of the small pelvis;
- returns the normal course of the lumbar vertebrae.
If you feel any discomfort, consult your doctor. The first thing to do at the first symptoms is to pay attention to: a bed (a wide selection of orthopedic mattresses to be selected individually), a pillow (may not suit you in size or softness), position during sleep, motor activity. At home, without a medical examination, osteochondrosis of the lumbar spine can only be treated with bed rest. Therefore, a visit to a doctor is mandatory. In the remission stage and the acute phase of the disease, different drugs are taken. In the last phase, drugs are used to reduce pain, free the nerves from vertebral mites, and eliminate inflammatory processes. Prescribe: - locks; - glucocorticoids; - chondroprotectors; - myolaxatives; - non-steroidal anti-inflammatory drugs (NSAIDs).

The last group of drugs, in addition to pain relief, combats excessive body temperature, edema and inflammation. Such funds can be: rectal, for internal use, injectable, external. Treatment of osteochondrosis of the lumbar spine usually begins with NSAIDs:
- Diklofenak;
- Piroksikam;
- ibuppofen;
- Himeculide;
- Hapoxy;
- Decketoprofen;
- Meloksikam;
- Aceclofenac.
The anti-inflammatory drugs on this list are various ointments, tablets, and gels. Some tablet NSAIDs have contraindications for people with ulcers or gastritis. Muscle relaxants relieve joint stiffness and involuntary contractions of the back muscles by temporarily reducing muscle tone. This group of drugs includes tizanidine, tolperisone hydrochloride. When there is an opportunity to save the intervertebral disc, chondroprotectors are prescribed, which should serve to restore the fibrous ring. The course of taking such a group of drugs is very long - at least 1, 5 months, and the results can be seen only after a year. They try to avoid the appointment of glucocorticoids, as they have side effects when taking them, as this group of drugs belongs to steroid hormones. They should be taken under the supervision of the attending physician with compliance with all prescriptions, since only a specialist knows how to cure lumbar osteochondrosis. An example of such a drug is hydrocortisone. Blockages are not medications in themselves, but they are a powerful local pain reliever. The technique is as follows: the introduction of an injectable analgesic (OI) or a combination of OI with a drug from the group of glucocorticoids in the area of pain. The blocks do not have medicinal properties, but they can be addictive, causing a loss of sensitivity to these drugs. If injected frequently, the muscles surrounding the injection may atrophy. Therefore, with the reduction of acute pain by this method of treatment, the patient is prescribed medications designed to restore damaged tissues, blood flow, and help improve the tone of nerve and muscle fibers. This:
- Chondroprotectors, which have a general strengthening effect on bone tissue, normalize the metabolism of cartilaginous tissues.
- Vitamins that help restore the patency of the nerves.
- Biogenic preparations that stimulate the body to heal itself;
- Vascular drugs that thin the blood to improve the nutrition of internal organs.
During treatment, along with the main intake of drugs, antidepressants are prescribed. Here's how to treat low back pain during acute pain relief:
- apply external warming, analgesic and anti-inflammatory agents;
- do special exercises for your back;
- go give yourself a massage;
- lead a back-friendly lifestyle;
- put on a belt corset when you exercise.
Massage, physiotherapy, physiotherapy and alternative treatments.
Comparatively inexpensive and effective methods for combating shock absorber degradation are physical therapy, massage and physical therapy exercises. A real massage can only be performed by a professional with medical education, so a simple visit to beauty salons is not suitable for patients. Each stage of the disease requires a different pressure and technique. With proper therapy, the muscle spasm disappears, the back muscle structure is strengthened, and the pain gradually disappears. Physiotherapy is applicable only in the process of attenuation of painful processes or when they are absent (to maintain the mobility of the vertebrae). Gymnastics is selected individually, depending on the age, the state of the person and the stage of development of the disease. The productivity of therapeutic exercises is directly dependent on the quality of performance and frequency: they must be performed systematically. It is recommended to rest at home, lying on your back, bending your legs, placing a small roller under the lumbar area. The healing process is monitored with the help of X-rays, tomographic studies. Physiotherapy treatments are prescribed during remission and exacerbation. Methods like:
- acupuncture. An ancient method of treating pain, based on the stimulation of acupuncture points with fine needles. The procedure relieves spasms, reduces pain, eliminates it completely, reduces tissue edema;
- ultraviolet radiation, which stimulates the body to absorb calcium;
- ampilpus, named after the corresponding device. The treatment procedure is as follows: the plates of the apparatus are fixed at the back and the corresponding therapeutic current with different parameters flows through the plates;
- laser therapy. Lasers relieve pain, heal, stop inflammation in the lumbar vertebrae;
- darsonvalization. The method is designed to improve blood circulation, dilate blood vessels, stimulate nerve endings;
- Phonophoresis treats with ultrasound, stimulating blood flow to the muscular part of the dorsal region.
Each method has its own contraindications. It is more difficult with traditional medicine. Official medicine does not yet recognize that the grandmothers of midwives know how to treat lumbar osteochondrosis. Therefore, if a friend advises you to apply compresses made with burdock broth, take pine baths, you should consult your doctor. For anesthesia, a method such as hirudotherapy is used, but leeches hide behind this name, so doctors recommend being careful with this method of treatment.
Surgical Troubleshooting
In some cases, it is no longer possible to do without surgery. With advanced intervertebral hernia, neurosurgeons use microdiscectomy. The operation removes the damaged disk. If there are no contraindications, doctors can perform a nucleoplasty, which has many advantages:
- Does not require cuts;
- The operation takes up to 30 minutes;
- No restrictions on surgical procedures.
Important. To maintain mobility of the spine, strengthen the muscles of the back, it is recommended to do yoga, swimming, Pilates. Running produces a shock load on the vertebrae, so at the first sign of low back pain, jogging should be abandoned.













































